Feet-Relief is supported by our audience. When you purchase through one of our links, we may earn a small affiliate commission. As an Amazon Associate I earn from qualifying purchases.Your cost is not affected.
Essential Guide: What To Do and Avoid for Diabetic Blisters
Blisters are a pain, but diabetic blisters can be a nightmare. If you’re one of the millions of people living with diabetes, you know how important it is to take care of your skin. In this article, we’ll explore what diabetic blisters are, what causes them, and most importantly, what you can do to prevent them from forming in the first place. So let’s get started!”
Diabetic Blisters
Diabetic blisters, though not commonly known, are a significant concern for individuals living with diabetes. These blisters, also known as bullous diabeticorum, can be quite uncomfortable and, in severe cases, lead to more significant complications. This article aims to provide a comprehensive guide on diabetic blisters, what to do and avoid, and how to manage these bothersome skin anomalies effectively.
Understanding diabetes and its complications is the first step toward effectively managing this chronic condition. Among the several skin conditions that can occur due to diabetes, diabetic blisters require immediate attention, primarily due to their potential to lead to severe infections if not adequately managed.
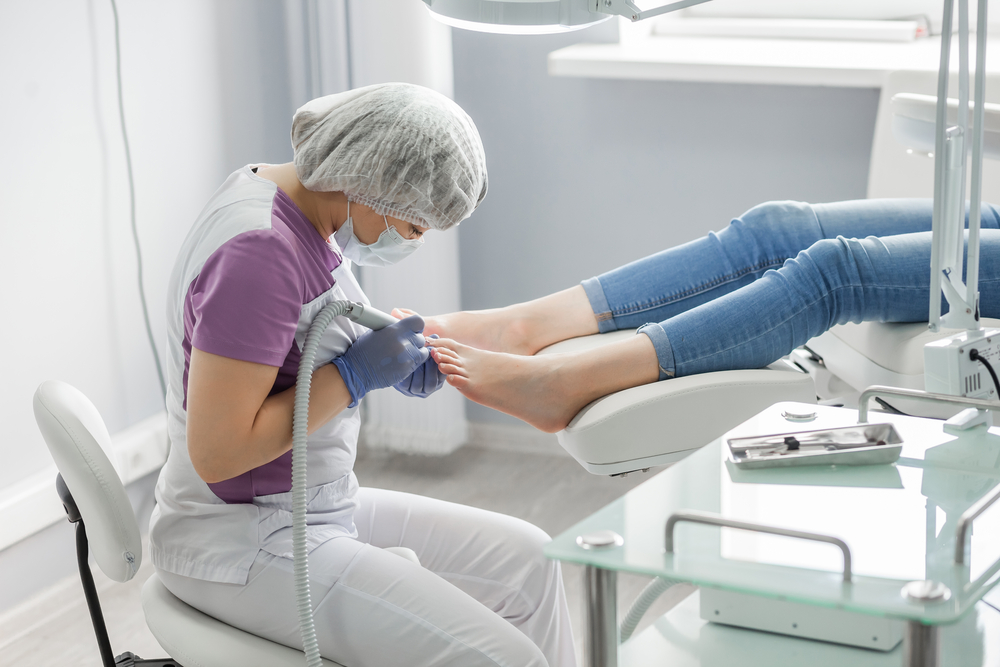
Diabetic patients skin complications
It is essential to note that diabetic blisters are relatively rare, with an incidence rate of approximately 0.5% among individuals with diabetes. Nonetheless, their presence can cause significant discomfort and distress, necessitating comprehensive knowledge of their management and prevention.
What are Diabetic Blisters?
Diabetic blisters are fluid-filled sacs on the skin’s surface, typically on the hands, feet, legs, forearms, and, sometimes, fingers and toes. They vary in size, from as small as a pea to as large as a nickel. In appearance, diabetic blisters resemble burn blisters and can occur singularly or in patches.
Unlike regular blisters, diabetic blisters are usually painless and have no redness around them, making them harder to notice. However, they can become quite itchy and often lead to infections if accidentally ruptured.
The exact cause of diabetic blisters is yet to be pinpointed by medical science, but it’s believed to be related to several common factors in people with diabetes. This includes poor circulation, nerve damage, and fluctuations in blood sugar levels.
The Link Between Diabetes and Blisters
Diabetes is a chronic condition that alters the body’s ability to use or produce insulin effectively, leading to elevated blood sugar levels. This long-term elevation in blood sugar levels can cause various health complications, including nerve damage and poor circulation, which are believed to play a significant role in the appearance of diabetic blisters.
The blisters are more common in individuals with diabetes who also have diabetic neuropathy (nerve damage due to high blood sugar levels). It is believed that nerve damage affects the skin’s structure and function, leading to the formation of blisters.
Moreover, poor circulation, another common complication of diabetes, can also contribute to developing diabetic blisters. Reduced blood flow to the skin can affect its health and elasticity, making it more susceptible to blister formation.
Causes of Diabetic Blisters on Feet
Several factors can contribute to the development of diabetic blisters on the feet. First and foremost, diabetic neuropathy plays a significant role. The nerve damage caused by elevated blood sugar levels can lead to numbness in the feet, making individuals less aware of injuries or pressure on the skin, which can result in blisters.
Secondly, poor circulation can also cause diabetic blisters on the feet. Reduced blood flow can lead to dry, cracked skin, which is more susceptible to blister formation. This is particularly true for areas of the body that experience frequent friction or pressure, such as the feet.
Lastly, uncontrolled blood sugar levels can also contribute to developing diabetic blisters. High glucose levels can damage the skin and affect its healing ability, leading to prolonged recovery times and increased risk of complications.
How Diabetes Causes Blisters
The exact mechanism of how diabetes causes blisters is not entirely known. However, it is believed to result from a combination of factors. These include nerve damage, poor circulation, and the effect of high blood sugar levels on the skin.
Diabetic neuropathy (nerve damage) is one of the most significant contributors, leading to numbness and reduced sensation in various body parts, particularly the feet. This can result in unnoticed injuries or pressure, contributing to blister formation.
Poor circulation, on the other hand, can lead to skin dryness and cracking, making the skin more susceptible to injury and blister formation. Elevated blood sugar levels can weaken the skin’s structure, making it more prone to blisters and other skin issues.
What to Do When You Have Diabetic Blisters
If you notice diabetic blisters on your skin, the first step is not to panic. It’s important to remember that while diabetic blisters can be a cause for concern, they are manageable with the right care.
Do not attempt to pop or drain the blisters, as this can lead to infections. Instead, keep the area clean and protected with a sterile bandage. If the blister is large or causing discomfort, seek medical attention immediately.
Manage your blood glucose levels as this can help in faster recovery and prevent further complications. Regularly monitoring and maintaining a balanced diet can help check your blood sugar levels.
What to Avoid When You Have Diabetic Blisters
If you have diabetic blisters, avoid any activities that can put pressure on the blister, as this can lead to rupture and possible infection. Avoid wearing tight shoes or gloves that can cause friction on the blister.
Do not try to pop or drain the blister, as this can introduce bacteria into the area and cause an infection. Similarly, avoid using over-the-counter medications or creams without consulting a healthcare provider, as some products can irritate the skin and delay healing.
Lastly, avoid poor blood glucose management. High blood sugar levels delay healing and increase the risk of complications. Therefore, keeping your blood glucose levels under control is essential.
Preventive Measures for Diabetic Blisters
You can take several preventive measures to reduce the risk of developing diabetic blisters. Firstly, manage your diabetes well. This includes regularly monitoring blood sugar levels, taking prescribed medications, following a balanced diet, and exercising regularly.
Maintain good hygiene and skincare.
Regularly clean and moisturize your skin, particularly the hands and feet, to prevent dryness and cracking. Be sure to dry your feet completely after washing or showering. Take special care to dry between your toes.
Wear comfortable, well-fitting shoes and avoid walking barefoot to prevent injuries and pressure on your feet. Avoid shoes with pointed toes, high heels, or tight-fitting shoes.
Regularly inspect your body for signs of blisters, particularly in areas with reduced sensation due to neuropathy. Early detection and treatment can prevent complications and speed up recovery.
Treatment Options for Diabetic Blisters on Feet
The primary treatment for diabetic blisters is to manage the underlying diabetes. This involves regularly monitoring blood sugar levels and appropriate adjustments to diet, physical activity, and medication.
If the blisters are large or painful, a healthcare provider may drain them in a controlled environment to reduce discomfort. However, this should not be attempted at home, as improper draining can lead to infections.
Topical antibiotics may be prescribed if there’s a risk of infection. In some cases, a physician may recommend using a protective dressing to reduce friction on the blister and speed up healing.
When to See a Doctor for Diabetic Blisters
You should see a healthcare provider if you notice any blisters on your skin, particularly if you have diabetes. It’s essential to seek medical attention if the blisters are large, painful, or located in an area that’s difficult to protect.
Additionally, if you notice signs of infection, such as redness, swelling, warmth, or pus, seek medical attention immediately. Similarly, if you have difficulty controlling your blood sugar levels, consult a healthcare provider, as poor blood sugar control can delay healing and increase the risk of complications.
Prevent diabetic blisters
Diabetic blisters, while rare, can be a significant concern for individuals with diabetes. However, proper care and management can effectively treat and prevent them. By understanding what diabetic blisters are and how they form, you can take proactive steps to prevent them.
Regular monitoring of blood sugar levels, good skincare practices, and early detection can significantly reduce the risk of diabetic blisters. Remember, when it comes to diabetic blisters, knowing what to do and what to avoid is the key to effectively managing diabetes. Include proper skin care and prompt medical attention when necessary.
Frequently Asked Questions
What do diabetic blisters look like?
These blisters usually show as white bumps with no red on or around them.
Should you drain diabetic blisters at home?
Puncturing the blister could lead to a serious infection. If it needs draining, see your doctor.
What if my blisters develop redness around them show swelling or feel warm?
Doctors recommend that you see your doctor or podiatrist immediately if these symptoms develop.
Do diabetic blisters hurt? Are they painful?
They usually don’t hurt at all. However, avoid opening them to prevent infection. And some foot blisters do become very painful and need medical treatment. If your blisters are painful, get medical care immediately.
How long do these blisters last?
If not opened, they normally heal within five weeks. However, that time may be longer if they are opened and become infected.
Can a blister turn into an ulcer?
Without treatment, some blisters can become ulcers and become a challenging health issue. If you think yours has, see a doctor for immediate treatment.
What heals foot blisters quickly?
The MayoClinic suggests applying an ointment such as petroleum jelly and covering it with a gauze bandage.
Amazon and the Amazon logo are trademarks of Amazon.com, Inc, or its affiliates.